Demographics of Neurological Face Pain at a Social Networking Website
(c) Richard A. Lawhern, Ph.D
March 16, 2012
This paper is cross-published online at "Giving Something Back" (http://www.lawhern.org)
and at "Living With TN" (http://livingwithtn.org), an online community within Ben's Friends
Abstract
A demographic analysis was performed on 1726 patient registration records from 55 countries, at a peer-to-peer social networking website focused on Trigeminal Neuralgia. While some demographic outcomes aligned with sources in medical literature, the patient demographic for first emergence of neurological facial pain was found to be younger than commonly noted in medical literature, by at least 14 years (median age slightly under 41 years, versus "sixth decade" or even "seventh decade" commonly reported). An analysis was performed to evaluate the potential impact of youth bias in this finding, due to the online and self-selected nature of the patient community; youth bias was not assessed as a significant factor in demographic results.
Over a fifth of patients in the demographic self-identified their pain as "Atypical" trigeminal neuralgia. Up to 80% of the demographic was female. In at least a quarter to a third of the demographic, the patient initially mistook their facial pain for a dental problem and saw a dentist as the first medical professional consulted. In less than a quarter of cases involving a dental practitioner, was the pain promptly recognized to be non-dental in character and the patient referred to a medical doctor. In a third of cases seen by a dental practitioner, the patient was treated for non-existent dental problems and pain did not resolve.
Introduction
Trigeminal Neuralgia (TN or "Tic Douloureux") is a relatively rare neurological disorder that produces intense pain in one side (or in a few cases both sides at different times) of the face. The disorder has sometimes been called "the suicide disease"[1],[2] and is widely considered to comprise the most debilitating form of pain known in medical practice[3]. TN is also relatively rare, with an estimated incidence rate of new cases on the order of 12 per hundred thousand population per year [4]. Some practitioners recognize two forms of the disorder. "Type I" or "Classic" TN is said to present as volleys of intense, brief, sharp, electric-shock jabbing pain, each jab lasting up to 90 seconds and volleys tapering off after one to two hours. "Type II" or "Atypical" TN pain is described as less-intense, constant 24-7 burning, boring, aching pain. [5] Distinctive medical mechanisms for these two forms of pain do not appear to have been clearly established in medical literature.
Many sources indicate that more patients are female than male. [6] Estimated age demographics vary by source. Some sources assert that Trigeminal Neuralgia most often first presents in the sixth decade of life[7],[8]. Other papers show a skewing of patient populations toward older age cohorts. [9]
Because of its relative rarity and overlaps in symptoms between TN and other neurological or dental problems, the disorder may present challenges to accurate diagnosis. [10] In a National Patient Registry created by the Trigeminal Neuralgia Association in 1999-2002, over 11,000 surveyed patients reported that they had been seen by an average of six different dental or medical practitioners before obtaining a diagnosis. Many physicians in general practice also relate that they have never personally seen a case of trigeminal neuralgia during 30 or more years of practice. [11]
In part because of the rarity of neurological facial pain and because of difficulties in obtaining accurate diagnosis and effective treatment, patients have in recent years increasingly turned to the Internet to find both information and mutual emotional support. Several on-line communities and Non Profit Organizations have grown up in response to this need. Prominent among these is the Trigeminal Neuralgia Association [12]. Other patient-to-patient communities having interests in chronic facial pain include the TMJ Association [13], Brain Talk Communities[14] and many others.
These on-line communities have significantly increased the visibility of relatively rare neurological disorders -- and on occasion called into question whether they are quite so rare as was once thought. For instance, in 1998 when the Trigeminal Neuralgia Association began to expand its on-line presence and patient information base, major Internet search engines such as Google and Web Crawler typically returned on the order of 4,000 "hits" for the term "Trigeminal Neuralgia". In March 2012, the same search produces over two million five hundred thousand "hits". [15]
One of the more recent entries among patient-to-patient mutual support sites is "Living With TN" (http://www.livingwithtn.org – a subsidiary community of “Ben's Friends”), operated since October 2008. The present paper analyzes the demographics of patients who have registered at the website, in an effort to address two questions:
1. Who gets face pain and at what ages?
2. How wide-spread are difficulties in obtaining accurate diagnosis and effective treatment
Demographic Analysis
The demographics of a substantial group of face pain patients were extracted from a download of "Living With TN" membership registration data, current as of February 5, 2012. Thirteen fields of membership data were employed to arrive at preliminary conclusions about the membership of the site and some of the outcomes of patient diagnosis and treatment.
Gender [male / female]
Location
Country
Zip
Age
Birthdate
Date joined
Last visit
Membership Type [patient, relative, friend, medical professional, admin, other]
Type of face pain [Typical TN, Atypical TN, Trigeminal Neuropathic Pain, Other]
Date diagnosed
Treatments you have undergone (member narrative)
Share your TN story with us (member narrative)
In several areas discussed below, membership records were updated from the original database to correct member entry errors and omissions.
Membership at Living With TN is world-wide, from 55 countries. The largest numbers of members come from the United States (1284), United Kingdom (156 ), Canada (73), and Australia (58). Categories of site memberships are indicated in Table 1 below:
Table 1: Types of Website Membership
Site Membership Categories Uncorrected Database Corrected database
Admin/Owners 4 5
Friends 11 23
Medical professionals/other 4 5
Relatives of patients 53 109
Member type not entered 725* 71 (narratives blank)
Patients - age unknown 8 8
Patients - age self-entered or estimated 1122 1695*
Patients supported by relatives (age known) -- 32**
Total member records reviewed: 1919 1919
[*] See "Corrections to the Member Database", below.
[**] 1727 Records were analyzed for the site demographic, including 32 records in which the registered member was a relative who reported the patient's age on first emergence of pain, or diagnosis of pain.
In the site demographic analysis, all records were removed for which a patient age at first emergence of pain was either not explicit in patient narratives, or could not otherwise be bounded by a member-entered date of birth or date of diagnosis.
Pain type(s) were directly entered by 969 members in the 1726 records analyzed for the demographic. None of these entries was corrected during database review, though it became evident that perhaps as many as 100 members were dealing with facial neuropathy rather than facial neuralgia
Table 2: Types of Pain -- Corrected Database (+)
Typical or Type I 244
Atypical or Type II 335 (98 patient narratives also mention "Atyp")
Bilateral pain 40 (from patient narratives)
Other / not sure 383 (includes 3 "trigeminal neuropathic pain")
No Type Entered 759
+ Does not sum: many patients entered multiple types in the “Type of pain” field.
Corrections and Additions to the Member Database
The database was reviewed to identify and correct the following types of errors or omissions.
- Although all members retained for the demographic had entered a date of birth for themselves or an age for someone whom they were supporting as a friend or relative, almost half of the site members originally did not identify whether they were patients, relatives or “other”. When "member type" was blank in the member registration data, patient story narratives and treatment history were scan-read to distinguish between patients, relatives, friends, site administration and medical professionals. When narratives provided circumstances or relationship words, member-type was added to the entry field originally left blank when the member registered. By this means, the number of records for which member category was unknown was narrowed from 725 to 71.
- In 1101 patient records retained for the demographic, an explicit date of diagnosis was entered by the member. When additional information on age of pain emergence was not available from patient narratives, the age of the patient when diagnosed was taken as an upper bound on age when pain first emerged. Given that many patients reported suffering for many years without getting a definitive diagnosis, this bounding probably introduces some upward bias in estimates of median age when pain first emerged.
- Patient narratives were reviewed for additional information that might permit estimation of an age when pain first emerged, when lower than the age of the member at registration. Narratives containing terms such as "my life", "first", “began”, “started”, "years" or “ago” were read to estimate the patient's age from circumstances recorded. Records of “Friends” or “Relatives” were also read, looking for age data on the patient being supported.
a. When an age was found in member narratives at which pain first emerged, this age was directly entered into a supplemental corrected age column of the database.
b. In 20 patient narratives, age of first pain emergence was qualitatively distinguished from the date of medical diagnosis by use of the words "for years" or "many years" in the patient narrative. When the phrases "for years" or "several years" appeared, a patient age at first pain emergence was estimated by subtracting five years from the date of diagnosis or the patient's age on registration. When the term "for many years" appeared, 10 years was subtracted.
- In 624 records of the demographic, a date of diagnosis was not entered by the member. Patient narratives were read to deduce the age at which pain first emerged. Wording was found in 391 patient narratives which allowed either a direct corrected age entry or a plausible qualitative estimate of patient age when pain first emerged.
- 76 records were excluded from the demographic because the patient and the member were different people and no patient age could be estimated from narratives. However, in most of these records, an approximate generational age relative to the member could be determined for the patient being supported. A bias check was performed to see if the demographics of this excluded group were substantively different from the group included in the demographic. No bias was found.
Gender Demographics
There were 1919 records in the uncorrected member database, of which 918 entered themselves as Female and 222 as Male, with 777 having made no entry. Records down-selected for the demographic analysis were those in which entered data was that of a patient or a relative acting on behalf of a patient whose age was known. A review was conducted of member user names during this down-selection, to identify female versus male user names. The resulting gender demographic is shown in Table 3, below:
Table 3: Patient Gender Demographic, Living With TN
Records entered or inferred as Female 1255 (80% of gender-attributable records)
Records entered or inferred as Male 302 (20% of gender-attributable records)
Records not attributable by gender 170
Total Records, Corrected Database 1727
Analysis of Patient Story Narratives and Treatments
The analyzed demographic sample omitted site administrators, medical professionals and members for whom the age of the patient could not reliably be determined. Of the 1726 patient records in the demographic, 1596 had text in the “patient story” and 1703 in “treatments you have undergone or will undergo”. In a few instances, text comprised “none” or “will fill in later”.
Text string searches were performed to estimate the number of instances in which key words appeared in the membership story or treatment history narrative fields. Word selection was guided by the author's 17-year experience as a patient advocate and webmaster for Internet chronic facial pain sites. The incidence of several key word strings is summarized in Table 3 below.
Review of patient narratives revealed that some members had a history of face pain from causes other than Typical or Atypical Trigeminal Neuralgia. There were 60 mentions of "MS" or "sclerosis" in patient stories, of which 20 were associated with a pending or confirmed diagnosis of the disease. There were 46 mentions of "tumor", 10 of "cyst" and 3 of "Chiari". 26 patient stories mentioned facial injuries from automobile accidents, assault, or other blunt force trauma.
Not surprisingly, a significant number of members had diagnosed themselves with trigeminal neuralgia or neuropathic pain by researching their own symptoms on the Internet. 82 patient records explicitly mentioned "research" and 30 more mentioned "internet". Several narratives also noted that multiple doctors and dentists had failed to diagnose Trigeminal Neuralgia ; some were actively resistant or dismissive to diagnosing the disorder in younger patients. By contrast, many patients reported a willingness on the part of dental practitioners to perform multiple extractions or root canals which did not resolve their pain -- despite an absence of evidence for abscess in dental X-rays, often over a period of years and on occasion involving the extraction of large numbers of teeth
Table 3: Keyword String Occurrences
Key word string Patient Stories Treatment Narratives
“dentist” 371 11
“dental” 157 17
(1 or both terms occur in a total of 469 patient records)
“tooth” 270 4
“teeth” 326 11
“canal” 145 9
“extract” 71 10
"pull" 95 4
“bite” 19 4
“TMJ” 73 8
“mouth” 114 1
1 or more among 8 above 631 36
(Keyword strings are combined below from patient stories, treatment history or both)
“migr” * 104
“effects” 168 (“side effects”)
"convul" 62 (anti-convulsive)
“tegr” 413 ("tegretol", "tegretal", "tegratol")
“carb” 215 ("oxcarbamaz.." or "carbamaz..")
“neuront” 161
“gabapen” 230
“trilep” 37 ("Trileptal")
“depr” ** 91 ("anti-depr..." or "depress")
1 or more of seven above 831
“surg” 542 (surgical, surgery, sometimes dental)
“proced” 107 (procedure, sometimes dental)
“MVD” 309
"vascu" 95 (vascular [de]compression)
“otomy” 149 (rhizotomy)
“radio” or "rf" 216 (radio frequency)
“knife” 179 (Gamma Knife, Cyber Knife)
"alcohol" 14 (alcohol rhizotomy)
"glycer" 41 (glycerol rhizotomy)
"balloon" 35 (balloon compression rhizotomy)
1 or more of 10 above 822
"Botox" 45
"bloc" 114 ("nerve block", "stellate ganglion block")
Notes to Table 1:
* “migr” = word root for “migraine” which is sometimes misspelled in patient-entered data
** “depr” appears in multiple contexts, including “anti-depressant” and “depressed”.
--- --- ---
Strong patterns stood out in the patient data with respect to outcomes of facial pain diagnosis or treatment by dental practitioners (dentists, periodontists, endodontists, oro-facial surgeons). One or more of nine dental terms or word roots appeared in 631 patient stories and 36 treatment histories. It was remarkable that many of the practitioners acceded to insistent patient demands for root canal or dental extraction -- despite a lack of X-ray evidence confirming abscess or other dental problems.
The terms “dentist” or “dental” or both, occurred in 469 member narratives. At least 174 additional patient records also indicated a history of dental work, described without these two words. Reading of patient story narratives revealed the following range of outcomes and contexts for dental terms:
1. In 60 of 469 patient records reviewed, mention of the terms "dental" or "dentist" was peripheral, imprecise, or context was otherwise unclear.
2. In 71 patient narratives, pain initially believed by the patient to be "dental" in character was evaluated by one or more dental practitioners, with a finding that the pain was not dental in origin. A practitioner then referred the patient to a family doctor, general practitioner or neurologist.
3. In 132 patient narratives, the patient had acute facial pain, saw dental practitioners and received neither a diagnosis nor a dental procedure. Patients in this group later saw a medical doctor or neurologist on their own initiative or at the suggestion of someone they knew. Several diagnosed themselves by performing Internet searches on their symptoms, before seeing a medical doctor. About 40 records included "online" referring to patient research or online support groups, or "research" or "self-diagnose".
4. In 154 patient narratives, the patient saw one or more dental practitioners and was treated with antibiotics, root canals, multiple dental extractions (sometimes at their own urgent request), TMJ therapy, bite correction, dental guards or major dental surgery. The terms "misdiagnose" or "mis-diagnose" appeared in 32 patient story narratives, and "unnecessary" in 14.
5. In 50 narratives, the patient saw a dental practitioner for routine dental work (cleaning, cracked tooth, crown replacement, other). Within hours to weeks after dental work was performed, the patient experienced extreme facial pain which they later believed was an outcome of something done by the practitioner.
Estimated Age at First Emergence of Face Pain
Median patient age in 1726 records 40
Average patient age 40.8
Median member age in 1726 records 44
Average member age 44.8
Number of patients 30 and younger 370 (21.4%)
Number of patients 60 and older 109
The youngest age at which pain was reported to have emerged was about 2 years old, and the oldest was 86. Half of all patient pain cases first presented between age 35 and 49.
Estimated patient age at first emergence of face pain in the corrected database is plotted in Figure 1 below, versus the number of patients in each year group. Shape of the statistical curve appears closely symmetrical about the median and Gaussian in shape. The mean and median closely aligned near 41 years of age. We do not see in this statistical curve, an assymetrical skewing toward older patients which is reported in some sources. [16]
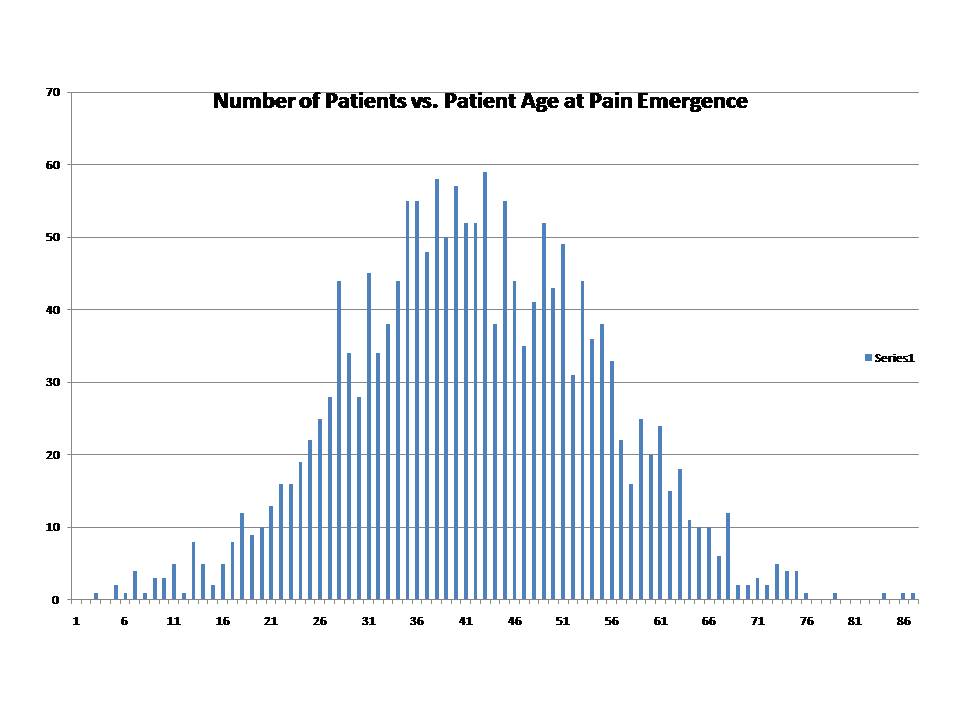
Figure 1: Patient Age at First Presentation of Pain, Living With TN
Potential Demographic Biases of Patient Self Selection
The patient sample reported in this paper was self-selected. Each member searched the Internet for key words, or was referred by someone else to "Living With TN", as a website that provides information and support for people with facial pain, neuralgia or neuropathy. The process of patient self-selection may potentially introduce two potential biases into demographic analysis:
1. Historically, Internet users have tended to be younger, more affluent and better educated than National populations overall. For some types of demographic analysis, this may introduce a youth bias in results.
2. People who join a patient-to-patient Internet support community as patients or close relatives are often dealing with bad outcomes of previous medical and/or dental diagnosis and treatment. Patients who have had a successful outcome from treatment are less likely to join or remain active in a support community focused on the needs of people in pain.
Youth Bias
Potential or significance for a youth bias in the computed demographic curve can be generally assessed by comparing the ages of the website demographic to US population and Internet user demographics. Particularly of interest are two related questions
"What is the expected value of numbers of people age 30 or younger in a group of 1726, randomly selected from a national population?" and
" What is the expected value of numbers of people age 60 or older in a group of 1726, randomly selected from a national population?"
By far the largest number of members at Living With TN reside in the US, UK, Canada, and Australia, all of which have similar national age demographics.
-- From 2010 population demographics in the US Statistical Abstract, the expected number people age 29 and below would be 707 in a sample of 1727 drawn at random from the US population (~41% of total US population, versus 21% seen in this demographic).
-- Expected numbers of people age 60 and above would be 310 (18% of total population, versus 7.7% seen in this demographic).
-- Median age in the US was 37 in 2010,[17] while the comparable figure for patients at Living with TN demographic is slightly older at 40.9. The median age of all Members in the demographic is 44.8, including 33 who were supporting patients as relatives.
In the demographics at Living With TN, both people under age 30 and over age 60 are under-represented relative to the US population as a whole. The relative rarity of trigeminal neuralgia in young people is well established in medical literature. However, as elaborated below, Internet user demographics do not appear likely to have significantly biased the mean patient age downward for chronic facial pain patients registered at Living With TN.
According to the Pew Internet and American Life Project,[18]
"Serious medical emergencies cut across all demographic groups [in the US] and seem to bump up interest in online health research. Fully 85% of internet users who experienced a recent medical crisis say they look online for any of the health topics named in the survey [high blood pressure, heart conditions, lung conditions, diabetes, and cancer], compared with 77% of internet users who have not had that experience in the past year."
Likewise in the US,[19]
-- Among American adults age 18-29, 94% use the Internet.
-- For adults 30-49, 87% use the Internet.
-- For adults 50-64, 74% use the Internet.
-- For persons age 65 and older, 41% use the Internet.
One can readily perform a significance check on the potential impact of under-representation among patients age 60 and older due to the online nature of the Living With TN community. In the patient population analyzed in this demographic, there were 134 patients older than age 60, with an average age of 64.9 years. If it is assumed that this group is under-represented by 50% due to non-use of the Internet by older people, then one may "add in" the missing cohort and compute the average age of the enlarged population. Addition of 134 members having an average age of 64.9 years to a base group of 1726 members with an average age of 40.9 years results in a demographic of 1860 members having an average age of 42.6 years.
Thus it may safely be asserted that even if patients over age 60 are under-represented by 50% at Living With TN, the "missing cohort" will have relatively minor bearing on conclusions drawn concerning the average age at which face pain first occurs. This effect is certainly not large enough to account for the 14-year difference between median age of patients registered at this website (41 years) versus the median age of new facial neuropathic pain patients expected from medical literature (mid-50's).
An effort was also made to ensure that records rejected from the demographic for lack of information on the patient, did not introduce an age bias in the demographic analysis. The age of members categorized as relatives or friends could be determined in 181 records and was an average of 41.6 years -- three years younger than the average age among members retained in the demographic. The generations of the members being supported by these friends and relatives could also be determined in 115 of the records. 31 patients were a generation younger than the member (sons, daughters, nieces), 43 were in the same generation (spouse, sibling or friend), 36 were in the next older generation (parent or parental in-law) and 2 were in the generation of grandparents. Allowing for an average difference between generations of 20 years, the estimated age of patients not incorporated in the demographic could be computed as 40.7 -- very similar to the 40.8 average age of patients in the demographic.
Negative Outcomes Bias
As noted in the introduction, Trigeminal Neuralgia and facial neuropathy in general comprise a very severe and life-altering form of pain. This pain and many of its medical treatments are known to be co-morbid with depression, though there seems to be little or no evidence that depression itself is a factor in causation. [20] Patients have likewise historically experienced great difficulty in having their pain recognized and diagnosed.
Multiple published papers document the success rates of neurosurgical procedures in reducing or eliminating the pain of idiopathic (classic or "Type I") Trigeminal Neuralgia. However, the author has found no broadly accepted estimates for surgical success in so-called "Atypical" ("Type II)[21] Trigeminal Neuralgia or in generalized trigeminal neuropathic pain due to trauma or organic disease. Although medication practice standards have been discussed for this class of disorders by organizations such as the International Association for the Study of Pain, the rates of treatment success, severity of treatment side effects and persistence of pain relief seem to be largely un-documented for common prescription medications.
In practical terms, the plausible result of factors summarized above may be that many people who join a web site like Living With TN are likely to be suffering from pain that is refractory to treatment. Website membership population will likely reflect "the tough cases". One may not extrapolate from patient experience in this sample to draw conclusions on the proportion of successful or unsuccessful outcomes for the larger group of all facial pain patients. However, it still appears valid to offer observations drawn from patient experience, recognizing that these insights apply most directly to patients who have had the most difficulty in a very difficult and disabling condition.
Demographic Observations
From analysis of patient age demographics, personal stories and treatment narratives, the following overall observations can be offered for the patient membership at Living With TN.
1. Although some medical literature sources suggest that median age for emergence of Trigeminal Neuralgia pain is “in the sixth decade” or even later, the median patient age at diagnosis among 1727 members at “Living With TN” is about age 41. Half of all recorded patient diagnoses at Living With TN occurred between ages 35 and 49. Patients younger than age 30 comprised a fifth of the demographic. Shape of the age statistic approximates a “Gaussian” distribution, with relatively few cases first presenting at ages younger than 15 or older than 70.
2. A substantial majority of membership at "Living With TN" is female (up to 80%). This demographic is even more concentrated in female members than is usually reported in medical literature.
3. Over half of registered patients either identified their type of pain as “Other/Don't Know”, or did not enter a type of pain in the registration field reserved for this entry. This statistic likely reflects the manner in which pain patients and their supporters find their way to a patient-centered interactive website such as “Living With TN”. As noted earlier, a sizeable majority of chronic condition patients now search the Internet to identify their own symptoms even before they are seen by a practicing dental or medical professional. Thus it is natural that many new members at Internet sites such as "Living With TN" will not know precisely what kind of pain they have when they register. They have come to the site in a search of such knowledge.
4. Of the 581 members in the demographic who entered a type of pain in the registration form, 336 identified themselves as “Atypical” Trigeminal Neuralgia patients. This 57% proportion cannot be confidently projected to the entire database without further analysis of narratives. However, even without projection, frequent mentions of chronic 24-7 burning, boring, searing facial pain strongly suggest that this type of pain is not "atypical" so much as simply "different" -- and significantly more difficult to treat -- than the jabbing electric-shock pain of Type I or "typical" TN. Moreover, many patients in the demographic experienced both forms of pain at the same time. Some had pain on both sides.
5. At least 819 patients in the site demographic had been prescribed one or more medications, with Tegretol and Neurontin the most often mentioned. One or more of nine keyword strings associated with surgical treatment occurred 822 times, with MVD (309) mentioned most often. Rhizotomy or RF ablation were mentioned in over 200 records and Gamma Knife or Cyber Knife in 179. Many patients indicated that more than one surgical procedure was performed and more than one medication prescribed. Severe medication side effects or medication intolerance were also frequently noted.
6. 650 member records contained one or more of the terms "tooth", "teeth", "canal", "bite", "TMJ", "mouth", "extract" or "pull". The terms "dental" or "dentist" occurred in 469 patient story narratives which were read and characterized in greater depth by the author. Fifty records mentioned the target terms only peripherally. For over half of patients who related having seen a dental practitioner, either no diagnosis was rendered or multiple dental procedures were performed without positive effect on the patient's pain. Patients later found their way to a medical practitioner on their own initiative after being seen by multiple dentists, endodontists, or dental surgeons. In less than a quarter of patient narratives did a dental practitioner inform the patient that their face pain was non-dental in origin and refer them to a neurologist or other medical doctor.
In the experience reported above, a general observation from medical literature is confirmed by patients at this website: in large numbers of cases, a dentist will be the first medical practitioner seen by a facial pain patient. From patient narratives at this social networking site, it appears that in many of these cases, the dentist will not recognize that a neurological disorder is the source of pain, and may perform unnecessary dental procedures under the assumption or belief that the pain is dental in nature -- or at the patient's urgent request. This finding is qualified by the reality that many symptoms of facial neuropathic pain overlap those of dental disorders, rendering diagnosis difficult and complex. Many MD general practitioners also have difficulty diagnosing facial neurological pain.
Recommendations
The observations above give support to three overall recommendations to the medical community.
1. From the reported experiences of 1727 patients, there is an evident need for greater depth in the training for both dentists and medical general practitioners, to better recognize and diagnose face pain of neurological rather than dental origins.
2. Practitioners who see pain patients need to be aware that they will see younger patients whose face pain may comprise trigeminal neuralgia or neuropathy. In a mixed population of face pain patients, some of whom have neuropathic pain from facial trauma of various types, 20% or more of those for whom the problem is non-dental in origin will be under 30 years old.
3. Many facial pain patients first experience debilitating pain near the peak of their earning capacity in their early to mid 40's -- rather than later in life, in or just prior to the retirement years. Thus pharmaceutical manufacturers and medical insurance companies may find it appropriate to reconsider research funding priorities for the effective treatment of neuropathic facial pain.
About the Author
Richard A. Lawhern is the spouse of a trigeminal neuralgia patient who has symptoms of both typical and atypical forms of this disorder, with pain on both sides of her face. His Ph.D. degree is in Engineering Systems (Dynamic Systems Control – UCLA, 1976). Since 1996, Dr. Lawhern has researched and authored multiple on-line articles and websites on behalf of chronic face pain patients, corresponding with over 3,000 patients, family members and medical professionals. Dr. Lawhern supports “Living With TN” (http://www.livingwithtn.org) as a site moderator, content author and resident research analyst.
References
[1] Wikipedia, "Trigeminal Neuralgia", 2012: http://en.wikipedia.org/wiki/Trigeminal_neuralgia
[2] Yam dela Cruz, "Salamat doc -- the Suicide Disease", ABS-CBN News, October 30, 2011, http://www.abs-cbnnews.com/current-affairs-programs/10/30/11/salamat-dok-trigeminal-neuralgia-suicide-disease
[3] Medicine.org -- Trigeminal Neuralgia, 2012, http://medicine.org/trigeminal-neuralgia-the-suicide-disease-may-be-the-most-painful-condition-known-to-medical-science/
[4] Koopman JSHA, Dieleman JP, Hygen FJ, deMos M, Martin Carola GM, Stirkenboom Miriam, "Incidence of Facial Pain in the General Population", Pain (2009)
[5] Jorge L. Eller, M.D.; Ahmed M. Raslan, M.D.; Kim J. Burchiel, M.D., "Trigeminal Neuralgia -- Definition and Classification", Neurosurgical Focus. 2005;18(5) © 2005 American Association of Neurological Surgeons
[6] Silvia RDT Siqueira, Manoel J Teixeira, and José TT Siqueira "Clinical Characteristics of Patients with Trigeminal Neuralgia Referred to Neurosurgery", European Journal of Dentistry, 2009 July; 3(3): 207–212. Web Reference: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2741192/
[7] University of Pittsburgh, Department of Neurological Surgery: http://www.neurosurgery.pitt.edu/imageguided/tn_facts.html
[8] Op Cit, Koopman et al (Mean patient age in demographic sample was 51.5).
[9] Op Cit, Silvia RDT Siqueira et al, see Figure I.
[10] Drangsholt, M, Truelove, EL,"Trigeminal Neuralgia Mistaken as Tempro-Mandibular Disorder", J Evid Base Dent Pract 2001;1:41-50.
[11] Lawhern, R.A. -- observations as co-author of the 2001 TNA Patient Registry survey forms and a member of the data reduction team [survey results unpublished].
[12] http://www.fpa-support.org/
[13] http://www.tmj.org/site/
[14] http://www.braintalkcommunities.org/
[15] Op Cit, Lawhern, R.A.
[16] Op Cit, Silvia RDT Siqueira
[17] Statistical Abstract of the United States, 2012 "Population - Estimates and Projections by Age, Sex, Race/Ethnicity" Table 7, Resident Population by Sex and Age.
[18] Pew Internet and American Life Project, "Who Gathers Health Information Online? -- Profiles of Health Information Seekers", February 1, 2011. http://pewinternet.org/Reports/2011/HealthTopics/Part-2/Adults-who-faced-a-recent-medical-crisis.aspx
[19] Pew Internet and American Life Project, "Who's Online? -- Demographics of Internet Users
[20] Jannetta, P.J., M.D. and the Medical Advisory Board of the Trigeminal Neuralgia Association, "Facial Pain Experts Establish a New Pain Classification", Knowledge Base of The Facial Pain Asspociation, 2011, http://www.fpa-support.org/2011/10/facial-pain-experts-establish-a-new-pain-classification/
[21] Jorge L. Eller, M.D.; Ahmed M. Raslan, M.D.; Kim J. Burchiel, M.D., "Trigeminal Neuralgia -- Definition and Classification", Neurosurg Focus. 2005;18(5) © 2005 American Association of Neurological Surgeons